What Every Person Should Know about Low Energy Availability & RED-S
March 2, 2021
By Lexi Moriarty, MS, RD, CSSD & Ashley Dimon, Sports Nutrition Volunteer
Depending on your circles, you may’ve heard low energy availability (LEA) RED-s (relative energy deficiency in sport), but you may not be sure exactly what they mean. So, I want to take a few minutes to break it down for you here!
Here are the top 5 things that EVERY active female (and male too!) should know about low energy availability (LEA) and relative energy deficiency in sport (RED-S).
What is Low Energy Availability?
Energy availability simply refers to how much energy (or calories) is being brought into the body and if it’s enough to manage everything the body needs to do on a daily basis. There needs to be enough energy to keep physiological processes going, activities of daily living, and exercise.
LEA or RED-S occurs when the body does not receive enough energy (or calories) to meet its daily energy needs.
To understand RED-S, we need to first remember the female athlete triad. The female athlete triad consists of three components: low energy availability, menstrual dysfunction and low bone mineral density. It refers to the interrelationship of low energy in the system, irregular or missing menstrual cycles, and the their resulting impacts on bone health.
The female athlete triad is so so important for active females to be aware of, BUT it completely leaves out two very important things. The first is that, bone health and reproduction (or menstrual cycles) are NOT the only systems effected by LEA. Second is that very similar variety of consequences can ALSO occur in males where this occurs. Enter RED-S or the term low energy availability (LEA), which encompasses ALL OF THE health and performance consequences that come along with this energy imbalance.
Who Can Be Affected by Low Energy Availability and RED-s?
Although research on RED-S and the female athlete triad mainly includes athletes anyone can experience LEA. The concept of low energy availability (LEA) can apply to all females and males, active or not active, who simply aren’t eating enough.
The important thing to remember is that this can be going on for a variety of reasons. LEA does not always occur with disordered eating, although disordered eating tendencies are common in LEA.
Some of the most common reasons for LEA other than disordered eating include:
- Low priority of eating
- A busy schedule with limited time to eat or availability of food
- History of disordered eating
- Low body fat
- Lack of knowledge about nutrition
- High levels of training and exercise
- A mismanaged weight loss program
Hormone & Bone Implications of Low Energy Availability
One of the most common and serious implications of LEA is its impact on hormone health. As a result of LEA, women tend to experience irregular or missing periods, and men experience symptoms of low testosterone.
While menstrual dysfunction, also known as amenorrhea, oligomenorrhea, or missing/irregular periods, isn’t uncommon in women, most women aren’t aware of its connection to LEA.
A regular period cycle is typically 21 to 35 days and ideally should last a minimum of 3-4 days. When there are fewer calories available to the body for energy, the body will skimp on the energy it puts towards systems, like reproduction, that aren’t seen as necessary for survival. For females, this almost always means their menstrual cycle and fertility will be impacted.
Irregular periods can occur in as many as 60% of recreational athletes. Up to 65% of athletes in some sports, especially those that idolize thinness like running, gymnastics, and dance.
The hormone levels in men can also be impacted by LEA resulting in low testosterone levels. Both menstrual irregularities and low testosterone levels have been linked to low bone mineral density in males and females. This can lead to increased risk for injury and osteoporosis (softening of the bone) at a young age.
There is of course other causes of irregular periods, hormone imbalances, and low testosterone other than LEA. Unfotunatly, there is currently no definitive test to identify when LEA is the cause. Through both personal experience and hearing my clients’ experiences, I find that doctors don’t discuss the potential of LEA enough with their patients. However it’s important to note that this is also a very new and developing area of research.
Other Signs & Symptoms of RED-s and Low Energy Availability
Although hormonal changes are often the most noticeable effects of LEA, it can effect a lot of other systems too. Your body wants to do anything that it can survive on a day-to-day basis. So, if there is less energy available for survival, high-priority systems will be prioritized. Your body will focus on your heart, brain, and lungs above all else.
As a result, other systems, like hair, nails, skin, immunity, optimal cognition, and digestion, will have less energy for use. Check out a few of the health and performance consequences below that were found during the more recent RED-S studies.
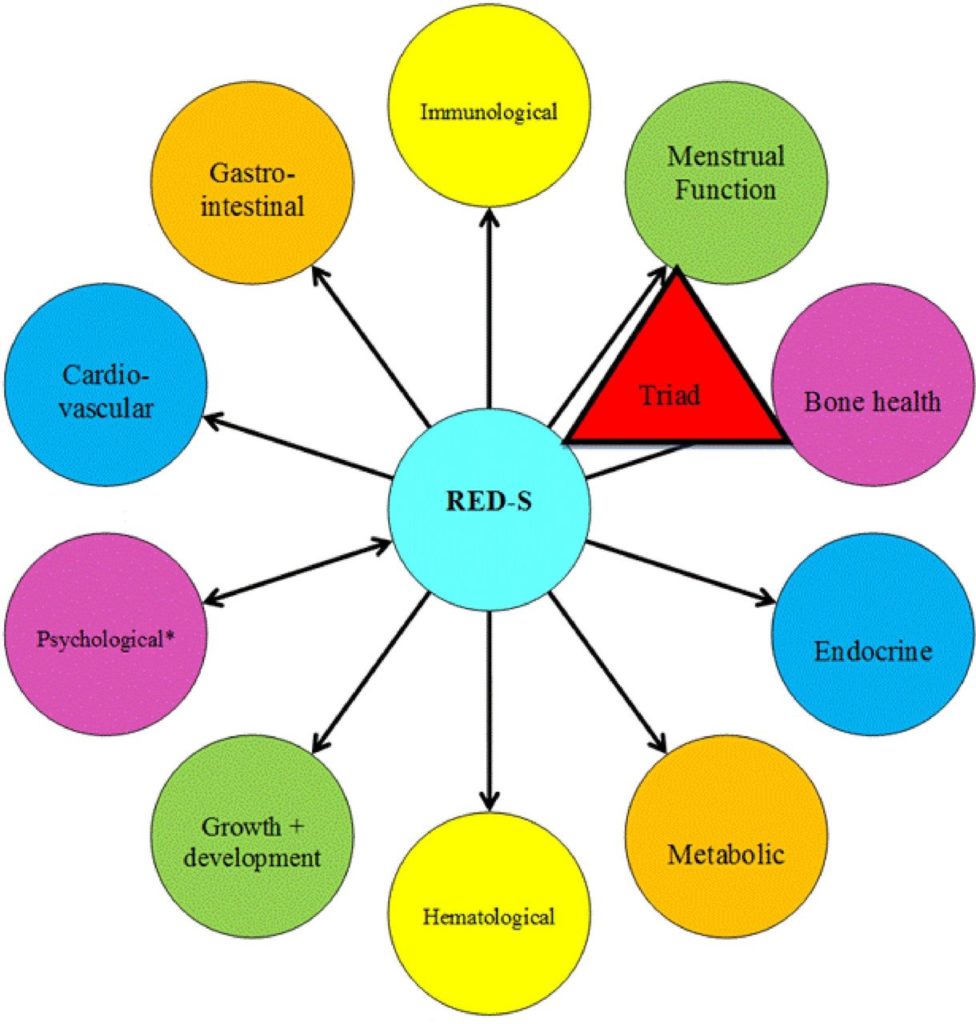
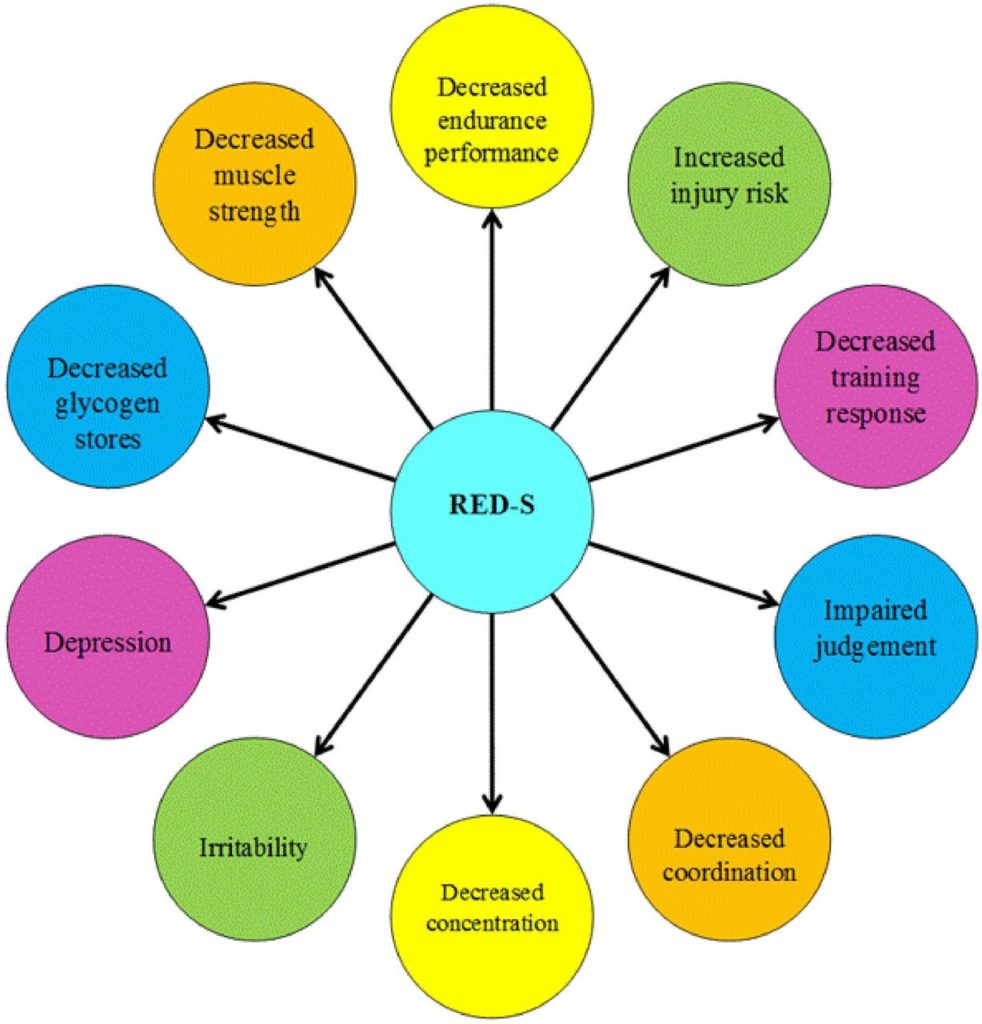
How are Low Energy Availabity and RED-s Diagnosed?
At this time, the best way to identify LEA as a factor in abnormal menstruation, low testosterone, or other questionable symptoms is by process of elimination. It’s important to rule out specific medical conditions and vitamin/mineral deficiencies early on in the investigation.
However, dietary and lifestyle changes to address LEA are often easy and risk-free. If energy availability issues are a concern for you, a nutrition assessment by a Certified Sports Dietitian can be an easy next step. A dietitian that specializes in RED-s and LEA will help you get your health and performance back on track.
References:
Mountjoy M, Sundgot-Borgen J, Burke L, Ackerman KE, Blauwet C, Constantini N, Lebrun C, Lundy B, Melin A, Meyer N, Sherman R, Tenforde AS, Klungland Torstveit M, Budgett R. International Olympic Committee (IOC) Consensus Statement on Relative Energy Deficiency in Sport (RED-S): 2018 Update. International Journal of Sport Nutrition and Exercise Metabolism. 2018; 28:316-331.
Mountjoy M. Relative Energy Deficiency in Sport Clinical Approach in the
Aquatic Disciplines. Aspetar Sports Medicine Journal. 2020;9:414-419
[…] Low energy availability results when energy intake isn’t enough to compensate for energy use. In other words, calorie intake is not enough to fuel body processes, daily activities, and exercise. As a result, an energy gap is created. Creating this gap is often the whole goal of low-calorie diets. Long-term, this gap in energy balance can result in gastrointestinal issues like gas and bloating. It can also cause irregular or missing periods, low energy levels, decreased training gains, and long-term cardiovascular, immune, bone and fertility issues unless corrected. […]
[…] you have not heard of RED-S, it is an acronym for Relative Energy Deficiency in Sport. RED-S was first introduced in 2014 with […]
[…] loss is a common symptom of relative energy deficiency in sport (RED-S). RED-S is a condition that can simply be defined as inadequate energy consumption leading […]
[…] Low energy availability (LEA) is one of the most common issues for active individuals that can negatively affect bone health. […]
[…] GI issues can sometimes be a direct result of underfueling or low energy availability. This can be a common occurrence among athletes or active individuals. Active people may eat less […]
[…] start experiencing negative effects. Health and athletic performance may be hindered by “low energy availability” or “relative energy deficiency in sport” […]
[…] can lead to conditions like RED-S, or relative energy deficiency. RED-S occurs when we expend more energy than we take in and can be […]
[…] practices can lead to decreased performance, fatigue, injuries, hormonal imbalances and more. I don’t know about you, but this sounds like OPPOSITE getting […]
[…] cutting out foods and overly focusing on low calorie options like fruit and veg, it can be easy to intentionally, or unintentionally undereat. On the other hand, some individuals may simply have a difficult time keeping up with the high […]